
How to know if you have Rectal Prolapse or a Rectocele
As a pelvic floor physical therapist, I work with many individuals seeking guidance on pelvic health concerns, and one common issue that often leads to confusion is the differentiation between rectal prolapse and rectoceles. Both conditions involve the descent of organs in the pelvic region, but they differ in their symptoms and implications.
Defining Rectal Prolapse
Rectal prolapse (sometimes called anal prolapse) is a condition where the inner lining of the rectum loosens, moving into the anus and sometimes slides out of the body, similar to a telescope. This protrusion, or prolapse, typically appears as a reddish mass as the inner lining of your rectum and anus are unfolded to the outside of the body. Most commonly this can be seen during bowel movements. However, if it does not retract after defecation it can stay out at all times
The 5 Most Common Rectal Prolapse Symptoms
There are several pelvic floor exercises that can help improve your sexual wellness and unlock the full potential of your orgasms. These exercises are gender-neutral and inclusive, ensuring that everyone can benefit from them as long as they’ve been vetted and approved by your healthcare providers.
1. Visible Mass
The most apparent symptom of rectal prolapse is the protrusion of the rectal lining through the anus, resembling a reddish mass or a fleshy lump.
2. Discomfort or Pain
Some individuals may experience discomfort, pain, or a sensation of pressure in the rectal region, especially during bowel movements.
3. Bleeding
Rectal prolapse can sometimes cause minor bleeding or mucus discharge from the rectum.
4. Incomplete Bowel Movements
Difficulty fully emptying the bowels may occur due to the prolapsed tissue blocking the rectum’s passage.
5. Incontinence
Rectal prolapse can contribute to fecal incontinence or leakage of stool.
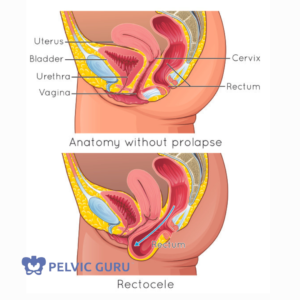
Defining Rectocele
Rectocele is a condition in which the wall between the vaginal canal and rectum slackens or loosens. Depending on the degree of new tissue length, this back wall will come into the vaginal canal and sometimes slide outside of the body. It is more commonly observed in people over the age of 60 who have a vagina/middle opening. Risk factors for rectocele include multiple births and vaginal or middle opening delivery.
The 5 Most Common Rectocele Symptoms:
1. Protrusion through the Vagina/Middle Opening
The primary symptom of a rectocele is the protrusion of back/posterior vaginal wall through the vagina/middle opening
2. Chronic Protrusion
With a rectocele, the rectal tissue often remains protruded and does not retract on its own.
3. Discomfort and Pain
Individuals with Rectocele often experience discomfort, pain, or a feeling of pressure in the vaginal/middle opening area.
4. Difficulty with Bowel Movements
Bowel movements may be challenging, and individuals may feel as though they can’t fully empty, have hard, compact stool, and may need to place their finger in the vagina or around their rectum to splint while completing a bowel movement.
5. Sexual Troubles
Since a rectocele is within the vaginal canal and at times outside of the vagina/middle opening, many people can struggle with pain, difficulty with penetration or orgasm challenges.
Differentiating Rectal Prolapse and Rectocele
Depending on the severity of the prolapse or the degree these tissues have moved out of place and if they remain out of place can determine the level of success with conservative treatment.
While both conditions involve the descent of pelvic organs, the key differences lie in the tissues involved and the location of the prolapse.
Rectal prolapse affects the inside of the anus and rectum moving outside of the body. On the other hand, a rectocele involves the tissue of the vaginal canal moving into and possibly outside of the vagina.
Physical Therapy for Rectal Prolapse and Rectocele
Pelvic floor physical therapy is an effective approach to managing both rectal prolapse and rectoceles. A qualified pelvic floor physical therapist, like me, can design a personalized treatment plan to address specific symptoms and improve pelvic health.
5 ways that pelvic floor physical therapy can help with both conditions:
1. Strengthening Pelvic Floor Muscles
Pelvic floor exercises can help reprogram your pelvic floor muscles. For both rectal prolapse and rectocele targeted exercises can improve the support around the rectal and vaginal openings. Additionally, working on coordination between breathing and strengthening of your larger muscles groups, like the hips, will limit increased pressure in the abdominal canister which can increase the degree of prolapse.
2. Educating on Proper Bowel Habits
Pelvic floor physical therapy can help you learn proper bowel habits and techniques to reduce strain during bowel movements. By adopting healthier habits, such as avoiding straining and establishing regular bowel routines, many pelvic floor physical therapy patients are able to prevent exacerbating rectal prolapse and rectocele symptoms.
3. Providing Biofeedback Therapy
Biofeedback is a valuable tool used to help patients gain better awareness and control over their pelvic floor muscles. Through biofeedback, you can learn how to engage and relax your pelvic floor muscles more effectively, improving the overall control of your pelvic floor.
4. Offering Lifestyle Modifications
Pelvic floor physical therapy can provide guidance on lifestyle modifications, such as fluid and fiber consumption, to support your pelvic health and alleviate symptoms associated with rectal prolapse and rectocele.
5. Behavioral Modifications
Pelvic floor physical therapists can assist you in implementing behavioral modifications such as lifting mechanics, posture considerations, and stress management techniques.
Start Healing Today
Let me give a word of encouragement: by working with a pelvic floor physical therapist, like me, to help heal your pelvic floor, resolving your symptoms of rectal prolapse and/or rectocele is possible.
If you’re looking for a pelvic floor physical therapist who’s ready to help you get the healing you deserve, you can either book a virtual session or in-person session with me to receive a specialized, unique-to-you treatment plan to get the healing you need.
Want to know what to expect from pelvic floor physical therapy? My e-book, How to Get the Most Out of Pelvic Floor Therapy, was created to help you learn the basics of the pelvic floor, how to find a pelvic floor specialist who’s a great match, what to expect at appointments, treatment possibilities, and more!
We’ll work together to create a personalized treatment plan tailored to your needs. I’ll guide you through exercises, educate you on proper techniques, and provide you with the tools and resources to continue your progress outside of our sessions. I always strive to create a safe and comfortable environment for my patients to ask questions, share concerns, and receive the care they need.
Looking for additional resources on pelvic health? My YouTube channel holds dozens of videos where I offer free pelvic floor training, yoga exercises, and more. My instagram page takes a little bit more of a light hearted approach while still providing educational content. And of course, if you have a specific pelvic floor subject you’re looking for more information on, a quick search of my blogs may give you the answers you need.
Some of the links on this page may be affiliate links. Laura Meihofer’s LLC is a participant in the Amazon Associates Program and others, as an affiliate advertising program designed to provide a means for sites to earn advertising fees by linking to products Laura organically uses and trusts. If you purchase a product through an affiliate link, your cost will be the same, but Laura will automatically receive a small commission. Your support is greatly appreciated and helps her spread her message!
Disclaimer: This blog post is intended for informational purposes only and should not replace professional medical advice. Consult a healthcare provider for personalized guidance and treatment options specific to your needs.








Sorry, the comment form is closed at this time.