
What You Should Know About Prostatitis
November is Men’s Health Month, so we are taking this opportunity to discuss an issue that affects those with penises. Natal men’s health and wellness, sexual health, and how these affect their quality of life are important. Read on to learn about a controversial men’s health diagnosis that, when misdiagnosed, can seriously affect the quality of life and comfort of an individual.
Prostatitis: A Common Prostate Issue (Or is it?)
Prostatitis is a hot topic and controversial diagnosis in the medical community that not all providers agree upon. I can say that I have treated many patients who were given this diagnosis, yet their tests and measures did not align with this judgment and resulted in unnecessary procedures, surgeries, and medications that did not help. When they finally found their way to me, it was clear that prostatitis was not the issue but pelvic floor muscle tension was.
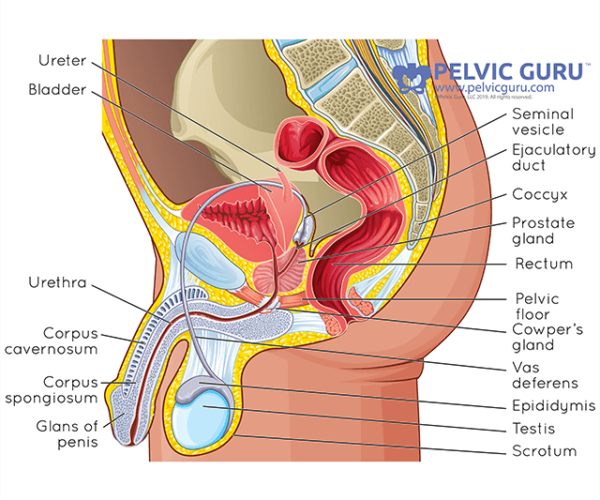
Prostatitis, simply put, is when the prostate gland becomes swollen or inflamed.
The prostate anatomy has also been covered in this post , but the purpose of this wondrous gland is twofold. Firstly, it creates the fluid that is mixed with sperm cells to make ejaculate fluid, and secondly, the muscles of the prostate help expel this fluid out during ejaculation. Due to its position just outside of the bladder, it lies within the layers of the pelvic floor muscles , so if an individual gets an infection within the prostate it can cause issues with other pelvic floor functions . However, there are actually four types of prostatitis.

Causes of Prostatitis
Here is where things can get tricky as the cause is oftentimes not very clear. Especially because the word prostatitis can refer to either a bacterial or nonbacterial issue. I recommend printing out the chart above and taking it with you to your provider so you can cross off and identify exactly which type they believe you have.
Bacterial prostatitis simply means you have bacteria in the prostate. There are many ways this can occur, and some include a bladder infection in which infected urine is captured within the prostate. Another way this could happen is by having anal intercourse without protection.
Nonbacterial prostatitis can occur for myriad reasons, including previously having a urinary tract infection, aggravated nerves, tight or inflexible pelvic floor muscles, and even previous pelvic floor injury.
Understanding that the causes of prostatitis can be very broad, the diagnosis process is extremely important.
Diagnosing Prostatitis
While other conditions may have a very clear diagnostic pattern or test prostatitis is oftentimes more challenging as it is about ruling out all of the other conditions. During this process of ruling out the other conditions, it helps your provider determine the type of prostatitis you have. This ultimately will help determine your treatment path.
It is important to note that if you are reporting concerns that may be considered a prostate issue oftentimes you will be sent to a urologist. This type of provider deals with issues of the urinary tract and reproductive tract that include the testicles and prostate. Your provider will first start with a thorough medical history to understand all of your symptoms and when they started. Then they will complete a physical exam which includes either a digital rectal exam or a digital vaginal exam to assess the prostate.
Next, they may run some or all of the following diagnostic tests:
- Urine tests: assessing for signs of infection
- Blood tests: assessing for infection and/or other prostate issues
- Post-prostatic massage: assessing for signs of inflammation and/or infection
- Cystoscopy: allows for examination of the urethra, prostate, and bladder
- Urodynamics: tests the strength of urine flow and helps to determine blockages caused by the urethra, prostate, or pelvic floor muscles
- CT scan: creates a 3D image that demonstrates any obstructions, infections, cysts, or tumors
- Sonogram: an ultrasound that can assess various structures, glands, and organs
Treatment Options
The course of treatment very much depends on what is causing the issue. If you have an infection versus muscular tension and/or nerve irritation, your treatment options will be very different. Here are some of the treatment options that your provider may recommend.
Medication Management
- Antibiotics
- Alpha-blockers
- Anti-inflammatory agents
Physical Therapy
- Manual pelvic floor therapy to your pelvic floor, hips, back or abdomen
- Home pelvic floor exercises in a program that includes breathing and stretching
- Awareness of your pelvic floor muscles to help change movement patterns
- Postural awareness to aid in proper body mechanics and toileting habits
- Dietary changes to minimize any bladder irritants or improper fiber consumption – Get your Elimination Program to Treat Yourself Here !
Prostatitis is often a condition that is poorly managed, though there are many things that can be done to improve someone’s symptoms and quality of life. So if you or anyone you know may be suffering from this, reach out and get the help you deserve.
If you have any questions about prostate and pelvic floor health, you can book a FREE 20-minute consultation HERE.
Or, if you’d like to learn more about all things pelvic floor, head over to Instagram! You can always reach out in the DM’s if you have any questions!
More content you may like:
Some of the links on this page may be affiliate links. Laura Meihofer’s LLC is a participant in the Amazon Associates Program and others, as an affiliate advertising program designed to provide a means for sites to earn advertising fees by linking to products Laura organically uses and trusts. If you purchase a product through an affiliate link, your cost will be the same, but Laura will automatically receive a small commission. Your support is greatly appreciated and helps her spread her message!






Sorry, the comment form is closed at this time.